You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Within a practice, balancing digital dentistry concepts with pre-digital "analog" dentistry is an evolving challenge. Although many dental offices are attempting to become 100% digital, they are more likely achieving only 90% while they continue to rely at times on traditional analog techniques. The primary question is: Between the two extremes-completely digital or analog-where is the practice, and where does the dental team want it to be? Would it be advantageous to integrate more digital systems? Are there areas where analog remains the better option, even within the changing dental landscape? To truly gauge the opportunities and make informed decisions, practitioners must take into account technical, efficiency, and cost-effectiveness factors. The multi-level relationships between digital and analog need to be assessed for the best fit for the practice.
To start, five questions about the current practice can help determine where it stands, and where a change might be worthwhile:
• Is the current system working?
• Would a change in technology significantly improve clinical results?
• If a change resulted in comparable clinical results, would the technology be more patient-friendly, giving more people access to care? Would it be more comfortable, efficient, or cost effective?
If indicated, a shift to more digital dentistry may be worth implementing, despite other challenges. Ironically, the tipping point-if there is one-for many practices may not come from the chair, but from the bench.
Laboratories Take the Lead
In their interactions with the dental laboratory, clinicians are already taking advantage of digital dentistry, even if it is not central to their office. Much laboratory work is now accomplished using digital workflow, CAD/CAM, and other relevant technologies. Even when using an analog fabrication technique for the restoration, the laboratory often still relies on a digital workflow, and even smaller, one-person laboratories are outsourcing work to milling centers.
Consider the process of fabricating a restoration. Clinicians' experience with milling restorations is typically with in-office milling units using very small blocks or with the aforementioned 3-D printers. However, at the laboratory, milling or printing takes place on a much larger scale and the process is vastly automated via digital scans, design software, and centralized production systems that permit a high volume of coincident processing.1-2 This milling technology has achieved demonstrable accuracy from both a manufacturing and a clinical perspective, ultimately benefiting the lab, the practice, and the patient.3-6
Thus, most dentists today live and work in a hybrid world: often the laboratory is digital, while the practice is analog or in transition, necessitating additional steps in the workflow. The more dental laboratories rely on digital data, the more important it is for dental practices to examine how diagnostic information is captured and communicated to the laboratories, whether through analog or digital technology-or a combination.
Capturing and Communicating Records
One of the first ways that dentistry entered the digital world was by moving away from traditional radiography. Although film and developing materials still exist, the majority of practices have made the transition to digital sensors and monitors.7 A clinician's choices for entry into digital imaging have expanded significantly.
A first-level digital integration that can be easily implemented, without intense technical experience, is digital photography, using an intraoral camera to capture images from many perspectives (tooth, smile, face). Previously, with film photography, if a photograph were missed or if the exposure were wrong, the patient was gone before a clinician realized the images would need to be retaken. Digital photography provides immediate results in real-time. The opportunity to gain instant feedback and continually adjust is invaluable to a productive workflow and superior results.8-10
Another advantage with digital images is more efficient storage and organization. Images can even be transmitted and saved over Bluetooth or Wi-Fi, which removes the need for a camera card to transfer images. This integration provides a streamlined system.8-10
The downside is mastering different camera hardware and designing a storage system that works with the practice software, retrieval systems, and storage needs to be maintained and backed up and secured.10 Another issue is the the need to secure transmission of sensitive medical information in and out of the practice. Secure communication is necessary to remain HIPAA-compliant and maintain patient confidentiality.11 Transferring digital data raises concerns that transferring analog data does not, especially when a clinician needs to transfer analog and digital data together.
Digital records are especially valuable when used to collaborate with a laboratory. The clinician can send images of preparations to the technician while the patient is still in the chair, even before impressions have been taken, to solicit feedback. The technician can provide input on the need for more taper or how accurate the margin appears. In addition, the images provide a humanizing element for the laboratory, showing the patient's face, eyes, hair color, smile, and lips, which provides a better sense of how to shape the esthetics.
As shown by the integration of digital photography, even small decisions can have significant impact on a dental practice. A simple choice, such as switching to a digital SLR camera for more sophisticated photographs, leads to using the device for videography as a dynamic piece of the treatment puzzle. As esthetic dentists transition from static photography to videography, the laboratory technician will be able to hear patients talk and see them move, gaining a better understanding of dynamic lip mobility. This level of laboratory communication advances collaboration and allows the dentist the freedom to work with laboratories unhindered by geographic location.
Next-Level Integration: CBCT, Digital Impressions
Adding cone-beam computed tomography (CBCT) into the practice enables a more advanced level of digital imagery. In addition, incorporating digital jaw tracking is moving dentistry closer to full replacement of the articulator. Clinicians will likely come to rely on a virtual articulator that combines records such as facial photography and videography with CBCT, intraoral full-arch upper/lower scanning, and digitized jaw tracking.12 Together, these tools create a 4D representation of the patient, revealing how the mandibular and maxillary teeth work together in real time.
CBCT is a classic example of the complex, evolving decisions required before acquiring and implementing advanced digital tools. When this technology first came became available, it was viewed primarily as an adjunct to implant dentistry.13 However, CBCT has now moved from the realm of implantology to broader applications. The technology can be used to diagnose at the level of the temporomandibular joints or to assess airways.7,14,15 In addition, it can be a valuable tool for orthodontics or endodontics, which demonstrates how it has moved from a niche application to a routine, general practice technology.14-16 After assessing their technology needs, some clinicians are choosing to replace digital panographic systems by investing in CBCT, taking advantage of a more advanced capacity to serve patients.
Similarly, digital impression systems' use in the dental practice has shifted from its earlier purpose. Initially packaged with in-office milling, digital impression systems have now been separated to allow for different purchasing choices to fit the practice. Introducing a digital scanning or impression system into the office can be a less complicated decision than incorporating in-office milling.
The options for digital scanning have advanced from the ability to scan only a quadrant to an entire arch of teeth quickly, as well as from only scanning bite records to scanning how the teeth are in maximum intercuspation. The computer can articulate the upper and digital models together. Furthermore, scanners have become smaller while moving to different file formats.17-19
Digital impression systems are growing in popularity: it is becoming more mainstream for practices to incorporate some form of digital scanning. Also of note is the ability to 3D print surgical guides in-house and integrate this with CBCT, which is invaluable for dentists who place implants.13,19 They can design the implant placement, create the guide, and send it directly to a 3D printer in their office. Other 3D printing options that are becoming more popular are occlusal appliances and nightguards, along with printing metal such as full-coverage gold restorations.20
Working a Hybrid System
Hybrid systems raise the question of compatibility and open architecture software.21 Clinicians must question if a piece of technology will integrate with systems already in use. Will the data gathered from the new technology integrate smoothly with current dental software and patient charts? Will the system run on the practice's existing network, or will it require separate computers, networking and/or storage devices? Beyond the practice, will the file formats work for the laboratory?
An example of extra steps need to adjust for incompatibility is working with physical articulators. Years ago, because they weren't interchangeable, if a clinician mounted a patient's model on an articulator, the entire articulator had to be shipped to and from the laboratory because they couldn't take the models off one instrument and place them on another and achieve accurate results. This situation improved when the instruments became more compatible and interchangeable across the board. Technicians could then see the same mounting that clinicians did. For incompatible digital systems, converting data back and forth adds extra steps to the process.
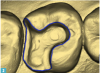
One common situation when analog is still used in the office (and digital in the laboratory) is when a clinician takes a physical impression to send to the laboratory, which then needs to digitize the data. The technician transfers analog to digital data by either physically scanning the impression or pouring the model from the impression and scanning it (Figure 1). For this dual analog/digital process, clinicians can use impression materials that improve the laboratory's ability to scan impressions. Materials that build upon VPS impression material afford greater accuracy when an impression is digitized, leading to more accurate digital data.22,23Clinicians can contact their laboratory and ask if impressions are being digitized or scanned, and choose their impression material accordingly, to facilitate the most accurate-fitting final restoration. If the laboratory is scanning the physical impression, the technician may need to spray the impression with a contrast material.22
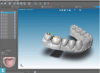
Digital data allows the laboratory to facilitate a design process integrated with either a milling or printing machine. For example, if the case is a crown and bridge, the technician works with software, tracing the margins of the preparation (Figure 2). The laboratory can also create digital wax-ups and models for restorations (Figure 3). The laboratory could also reverse the process, creating models from digital data. For example, if a clinician uses an intraoral scanner, the laboratory is receiving pure digital data with no physical impression. However, if the technician sees a reason to create a physical model, the process will have to move from digital to analog. The three modalities for this are: 1) a milled model, by carving the model from a plastic or PMMA material; 2) stereolithography, an older technology in which a vat of resin is cured in very precise layers to build a model up; or 3) the most state-of-the-art modality, 3D printing.24
The Digital Highway
Digital data has become the preferred workflow between practices and laboratories. One advantage is the ease of sending data through file sharing, which eliminates the need for boxing and shipping, along with the concerns of lost shipments or extreme temperatures ruining bite records and impressions. The built-in feedback system is also extremely beneficial in helping dentists evaluate and improve their work. When they look at preparations on a computer screen, they will either notice what could be improved.
There are two ways to transfer digital data to the laboratory: 1) intraoral scanning or a digital impression system; or 2) a box scanner in the practice. Including a box scanner in the practice is an efficient way for clinicians to interface between analog and digital systems. Once a physical impression has been taken, it can be scanned, digitizing the data for the laboratory. A clinician can take that impression and start making the provisional, the scan does not have to be completed immediately. This creates a workflow where in between patients, a clinical assistant can take an impression and proceed to set up a patient's case, then complete the scan and send it to a specific laboratory along with the prescription. One of the greatest advantages is being able to review the digital model as a means of gathering feedback. From an economic perspective, a box scanner may also be more feasible for a dental practice than an intraoral scanner.
There are aspects of taking a physical impression that are technique sensitive, and similar concerns for digital impression systems. Dentists may use intraoral scanners most often for their single-tooth dentistry, but for more advanced dentistry such as larger veneer cases or an entire quadrant, they may prefer to switch back to analog. Other dentists use a digital scanner for full crowns, but not for partial coverage. There is a learning curve associated with digital dentistry, and clinicians must feel comfortable with their skills.
How does a clinician decide between all the different intraoral scanners and digital impression systems on the market? A dependable first step is to physically interact with the technology and get a feel for the equipment. From this, clinicians can determine if the system will fit in the operatories or if they like the shape and weight of a handpiece. Other considerations are the the sensitivity of the camera, commitment to open architecture, and hardware and software interface. Is the user interface intuitive, friendly, and relatively simple to understand? In addition, although clinicians are often the ones buying the technology, they may not actually operate it. Consideration should be placed on whether assistants can "test drive" the system and decide if it is intuitive.
Making the Move
Now more than ever, the practice of dentistry is a hybrid of digital and analog along a wide spectrum of combinations. All of the many systems and technologies that have been discussed so far are not in fact "the future of dentistry"-they are already in use, although not completely entrenched. In the meantime, before new technology becomes more widely used, dentists will continue to practice with a foot in both worlds. Fortunately, excellent systems have been designed to navigate the ground between analog and digital, giving clinicians the time to decide when and where to incorporate more digital technology.
For example, with the ability to integrate analog data from an articulator into a digital articulator, clinicians have the power to evaluate how the soft tissue relates to the skeletal, and how that relates to the teeth, while visualizing all the functional and parafunctional interactions (Figure 4). As a result, clinicians can now design restorations to fit within the soft tissue, from a functional perspective.
As practitioners continue to assess their technology requirements, laboratories continue to be a valuable resource. Understanding their protocols and becoming part of the laboratory's digital workflow can increase cost effectiveness, efficiency, and quality of care in a dental practice. On the whole, clinicians have many options for expanding the amount of dentistry done with a laboratory in a digital space or streamlining their own in-office systems, and these options continue to advance.
Finally, an additional, important benefit of digital innovation is that it continues to engage practitioners, as they have increasing opportunities to learn different techniques for their practice and patient care, while gaining new insight into their workflow and expanding their perspectives on the frontiers of oral health.
REFERENCES
1. Battersby J. CAD/CAM - the end for dental labs or a new beginning? Dentistry IQ. May 6, 2014. Available at: https://www.dentistryiq.com/articles/2014/05/cad-cam-the-end-for-dental-labs-or-a-new-beginning.html. Accessed June 18, 2018.
2.Beuer F, Schweiger J, Edelhoff D. Digital dentistry: an overview of recent developments for CAD/CAM generated restorations. Br Dent J. 2008;204:504-511.
3. Sailer I, Feher A, Filser F, Gauckler L J et al. Five year clinical results of zirconia frameworks for posterior fixed partial dentures. Int J Prosthodont. 2007; 20: 383-388.
4. Tinschert J, Natt G, Mautsch W, Spiekermann H, Anusavice K J. Marginal fit of alumina- and zirconia-based fixed partial dentures produced by a CAD/CAM system. Oper Dent. 2001; 26: 367-374.
5. Vult von Steyern P, Carlson P, Nilner K. All-ceramic fixed partial dentures designed according to the DC-Zirkon technique. A 2-year clinical study. J Oral Rehabil. 2005; 32: 180-187.
6. Luthardt R G, Holzhuter M, Sandkuhl O et al. Reliability and properties of ground Y-TZP-zirconia ceramics. J Dent Res. 2002; 81: 487-491.
7. Farman AG. Digital radiography in dental practice. Inside Dentistry. 2016;12(11):26-27.
8. Desai V, Bumb D. Digital Dental Photography: A Contemporary Revolution. Int J Clin Pediatr Dent.2013;6(3):193-196.
9.Mladenovic D, Mladenovic L, Mladenovic S. Importance of digital dental photography in the practice of dentistry. Sci J Faculty Med in Niš. 2010;27(2):75-79.
10.Terry DA, Snow SR, McLaren EA. Contemporary dental photography: selection and application. Compend Contin Educ Dent. 2008;29(8):432-436.
11. Laskin B. Obtaining, storing, and transmitting patient files. Inside Dentistry. 2016;12(7):92-93.
12. Koralakunte PR, Aljanakh M. The role of virtual articulators in prosthetic and restorative dentistry. J Clin Diagn Res. 2014;8(7):ZE25-ZE28.
13. Surapaneni H, Yalamanchili PS, Yalavarthy RS, Reshmarani AP. Role of computed tomography imaging in dental implantology: an overview. J Oral Maxil Radiol. 2013;1(2):43-47.
14. Serota K. Cone beam computed tomography: how safe is CBCT for your patients. Dental Economics. 2011;101(1). Available at: https://www.dentaleconomics.com/articles/print/volume-101/issue-1/features/cone-beam-computed-tomography-how-safe-is-cbct-for-your-paitents.html. Accessed June 17, 2018.
15. Buchanan A, Cohen R, Looney S, et al. Cone-beam CT analysis of patients with obstructive sleep apnea compared to normal controls. Imaging Sci Dent. 2016;46(1):9-16.
16. Tally T. AAE/AAOMR recommendations for the use of CBCT in endodontics. Inside Dentistry. 2017;13(9):40-47.
17. Ehrlich T. The next level of digital impressions. Inside Dentistry.2016;12(3):
18. Antenucci E. Dental impressions: maturity of imaging technologies driving shift from physical to digital. Compendium. 2018;39(3):
19. Gallucci GO, Lee SJ. Digital vs conventional implant impressions. Efficiency outcomes. Clin Oral Implant Res. 2013;24(1):111-115.
20. Dawood A, Marti Marti B, Sauret-Jackson V, Darwood A. 3D printing in dentistry. Br Dent J. 2016;219:521-529.
21. Poss S. Digital versus traditional impressions: an objective discussion. Compendium. 2014;35(6):384-385.
22. Brown C. Making a new impression. Inside Dental Technology. 2011;2(4):60-63.
23. Perakis N, Belser UC, Magne P. Final impressions: a review of material properties and description of current technique. Int J Periodont Restor Dent. 2004;24(2):
24. Stover J. 3D printing: technology and fabrication of models in-lab. J Dent Technol. 2018;35(1):36-42.