You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
More patients are seeking cosmetic dental treatment than ever before. While many options are available to suit various needs and expectations,1 patients often have concerns regarding restoration durability, clinical procedures, finances, anesthetic injections, and removal of healthy tooth structure to enhance their smiles. Patients are requesting that their cosmetic alterations be completed in the most conservative and minimally invasive manner possible, so they have the option to consider other treatments in the future.2 As a result, increased patient expectations necessitate in-depth treatment planning and long-term conservation of maintainable natural tooth structure.3
Many of these issues can easily be addressed with direct composite restorations, which permit changes in tooth shape, size, color, and inclination.4 Direct composite restorations are cost-effective5 due to the elimination of laboratory fees. In addition, they are minimally invasive, provide significant esthetic improvements to a patient’s smile,6 and can be easily repaired. Also, there is usually no need for anesthetic injections.
Direct composite restorations also represent valuable selling points for dentists, particularly for patients opposed to indirect restorations. However, choosing between direct and indirect restorations should be based on an understanding of how many teeth are already treated and will need to be treated to enhance the smile.7 Therefore, knowledge of what components of a smile must be examined, as well as the numerous restorative issues that direct composite restorations can effectively resolve, are the foundation for conservatively transforming smiles.
Smile Analysis
Specific aspects of a smile are evaluated during a smile analysis. One essential aspect is whether a patient’s full smile follows the lower lip. A smile that is balanced with the lower lip is considered more pleasing. It has been observed that the absence of alignment between the lower lip and the edge of the maxillary incisors detracts from smile esthetics in frontal and lateral views.8
Upper incisor inclination also affects smile esthetics in the profile view,9 as do gingival margins. Most orthodontists and dentists prefer the lip elevation to stop at the gingival margins of the maxillary incisors but note that some gingival display is acceptable and often esthetic.8,10-12
Therefore, maintaining perfect symmetry at the gingival zeniths is not always necessary for the smile to appear pleasing. Slight variations are common among different individuals and are sometimes desired. An esthetic smile can be obtained as long as the anterior gingival line is comparatively horizontal to the horizon and approximately symmetrical on each side of the midline.13
Dental and facial midlines also factor into smile attractiveness. A high percentage of orthodontists, dentists, and laypeople noticed discrepancies of 2 mm or more between the dental and facial midlines. As the gap increased, the smile’s attractiveness became progressively less esthetic.14,15
For an ideal smile, the incisal embrasures from the central incisors to the canines should gradually increase in size. A lack of increase in depth and variation causes the teeth to appear boxy. Conversely, if the embrasures are too deep, the teeth will look unusually pointed.16 Incisal embrasures play a functional role in the masticatory system by allowing the mandibular teeth to clear the maxillary arch excursively. Therefore, altering incisal embrasures to achieve an esthetically pleasing smile should be carefully considered. Disproportionately altered incisal embrasures can result in chipping and breakage.16
Tooth shade, opacity, and translucency, all of which affect the esthetic appearance of a smile, tend to be important to patients. However, two teeth that are the same shade but have different textures will not blend well. Texture should not be overlooked when completing restorations in the smile zone.
Finally, while dentists can effectively alter these aspects through restorative measures, they may not have complete control over the patient’s papillary heights. Papillary heights and tissue position strongly influence tooth form and require careful evaluation. A reduction in papillary height is generally rated less attractive.17
Defining an Attractive Smile
Although smile design has generally accepted parameters, it is not an exact science. Dentists must rely on clinical judgment, patient expectations, health of existing tooth structure, and any other limiting factors.7 As previously noted, dental and facial midlines affect smile esthetics. Facial and dental midlines are estimated to match in approximately 70% of the population.18 However, research shows that the maxillary and mandibular midlines are symmetrical in only 25% of the population.18 While not essential, achieving coincident mandibular and maxillary dental midlines may be a key objective in creating an esthetic smile.14
Many patients consider smile makeovers to restore their smile to the proper proportions, because their teeth can become disproportionate through aging. Most commonly, tooth wear occurs on the incisal edge, making teeth shorter.19 Teeth also wear in a mesial-distal direction and erode on the facial. The dentist can effectively change tooth size and proportion through concentrated treatment planning and restorative efforts, providing patients with significantly enhanced smiles and occlusal schemes, if necessary. Mesiodistal and inciso-cervical crown dimensions and width-length ratios are considerations when designing a smile.19
Tooth brightness is an important component that determines their color and attractiveness. Many people prefer bright teeth. To determine the appropriate brightness of a patient’s teeth, it is generally accepted to replicate the whiteness of their eyes. Understanding the nuances of color (eg, the higher the chroma, the lower the value; brighter teeth appear larger and closer) aids in understanding what is too white. If the maxillary central incisors are too bright, they will appear too big. Appearance and reality can differ when relying on color illusions to create necessary effects; translucent shades in interproximal areas make teeth appear narrower. Opaque shades in the interproximal areas make teeth appear wider.20,21
The Role of Direct Bonding in Smile Enhancement
Direct composite restorations could be used to a greater extent for a number of esthetic restorative smile design cases, especially when patients request smile enhancements with minimally invasive procedures. Therefore, it benefits clinicians to examine the state of the patient’s existing dentition and gingival architecture, in addition to the overall smile esthetics.21 Occlusion and function should also be addressed, as bruxing, parafunctional habits, and occlusal pathology could contraindicate direct composite restorations.7 While not all smile transformations should be accomplished through direct composite restorations, today’s composites provide predictable clinical function and esthetic results when used for carefully selected indications.7
Using direct composite restorations allows dentists to alter myriad aspects of a patient’s dentition without compromising natural tooth structure. Direct composites have been used to treat caries, lengthen teeth, mask dark or discolored teeth, and repair fractured pontics.22 They have also been used for other indications, such as closing a diastema when no preparation of tooth structure is needed and the procedure calls for the most conservative treatment required.23 Based on the optical properties demonstrated by modern composite materials, they can be used for anterior restorations, even in cases involving fractured teeth.24
Newton Fahl Jr, DDS, has frequently documented his success with direct composites in numerous publications, suggesting that a combination of materials and technique is a prerequisite for predictable and lasting results.25,26 Regarding durability, Fahl sees direct composite restorations providing a lifespan of 10 to 15 years, on average.27 Studies comparing the fracture strength of direct and indirect composite laminate veneers found no comparable differences.28
The difficulty performing direct composite restorations that some clinicians may experience results from insufficient knowledge and training.27 Hands-on training provides dentists with an effective advantage when offering esthetic services to patients.27 Dentists who have performed composite restorations are familiar with which bonding systems to use and how to properly treat dentin and enamel. Once experienced with choosing the most appropriate approach to take for the remaining steps, direct composite placement can be perfected with continued performance. Mastering this technique allows dentists to produce direct composite restorations that are functionally sound, minimally invasive, and esthetically pleasing.28
Direct composite restorations can also be profitable. Fahl resolved the profitability issue by establishing patient responsibility for laboratory fees. This system allows him to charge the same for direct and indirect veneer restorations.27 Due to the potentially time-consuming nature of placing direct composite restorations, adjusting fees according to the length of the procedure is also an option.
Direct composite restorations allow clinicians to preserve the integrity of the natural tooth structure, a crucial service to patients who are unwilling to undergo invasive procedures to correct minor defects that are apparent in their smiles. Conversely, this restorative procedure enables clinicians to provide a conservative alternative to patients requesting more extensive alterations, of which they may not realize the inherent risks (eg, long-term consequences of removing sound tooth structure, future endodontic and periodontal problems).7
Material Selection
Material selection is often dictated by the location of the restoration in the mouth. Posterior restorations require strength to withstand chewing, grinding, and bruxing, while anterior restorations necessitate a material that provides strength and esthetics or possibly esthetics only, depending on which tooth is restored. Often, a combination of materials is best to ensure success.
Microhybrid and nanofilled composites are two of the most common materials used in direct restorations. Microhybrid composites have been used for anterior and posterior restorations for more than a decade, as they demonstrate excellent physical characteristics and improved handling.29 They are also noted for their superior tensile strength, fracture resistance, improved abrasion resistance, low coefficient of thermal expansion, and reduced polymerization shrinkage.30 However, microhybrid materials exhibit poor polishability and a need for maintenance of polish over time to sustain an esthetically pleasing appearance.23
Nanofilled composites are also ideal for direct restorations. These materials exhibit similar mechanical and physical properties to those of microhybrid composites, but provide better results in terms of polish and gloss retention.31
The material of choice for this case was a nanohybrid composite optimized for anterior restorations. Although not as strong as the firmer nanohybrid composite from the same family, which consists of prepolymerized fillers ranging from 5 nm and 20 μm, the nanohybrid chosen for this case consists of fillers between 5 nm and 5 μm, providing more luster and better polishability for anterior restorations. For a restoration in the esthetic zone, depending upon its function and location, esthetics may prove more important than strength.
Case Presentation
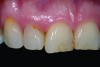
A 60-year-old female presented with worn incisal edges, discoloration among her maxillary teeth, and a reverse smile line that did not follow the curve of her lower lip (Figure 1). She also demonstrated receding gingiva on tooth No. 10 that created gingival disharmony in her smile. She was displeased with the overall appearance of her anterior teeth. However, the patient was uninterested in pursuing the more invasive surgical and restorative recommendations she had received from other dentists (ie, tissue graft, extraction, implant placement) that would have balanced the gingival display throughout the esthetic zone. She was opposed to removing any more tooth structure than was necessary, and her primary concern was for correcting the appearance of teeth Nos. 8 through 10.
Therefore, a treatment plan was discussed with the patient that would enhance the overall color harmony among her maxillary teeth. The treatment would also create a more balanced shape, length, and proportion among the anterior maxillary teeth, without the need for extraction. The patient agreed to first undergoing at-home vital tooth whitening, followed by direct composite restorations on teeth Nos. 8 through 10.
Clinical Protocol
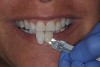
Impressions were taken and a model was made. While the patient performed at-home bleaching, an enhanced wax-up was created. The next appointment involved obtaining patient approval of the enhanced wax-up and performing a shade mock-up. As instructed, the patient discontinued bleaching 2 weeks prior in order to allow rehydration before composite layering. After bleaching, the tooth shade was determined to be between A1 and OM1 (Figure 2).
The direct composite material of choice was a nano-hybrid composite ideal for anterior restorations due to its polishability. In this case, especially for the facial aspect of tooth No. 10, which did not require additional strength, the location of the restoration dictated that the material’s optical properties, esthetics, and polishability supersede strength.
To perform the mock-up, the composite was first applied to the tooth without etching or applying adhesive. The selected composite was applied in a manner that would achieve the desired A1 shade. First, an opaque layer of 10% OLC was applied and light-cured, followed by 70% shade A1 composite for the base body shade that also was applied and light-cured. Because the patient presented with calcifications, white modifier was applied and layered over with 20% CL enamel composite for depth, which was then cured.
The oxygen-inhibited layer was removed with a bur, with care taken not to remove the surface or elicit a color change. Polishing was completed using a silicone occlusal brush at 10,000 rpm. Because the composite restoration had not yet been bonded, it was removed and the layers were examined. The mock-up was completed similarly for teeth Nos. 8 and 9.
Direct Composite Placement
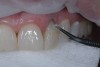
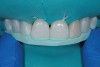
Prior to placing the definitive direct composite restorations on teeth Nos. 8 through 10, the teeth were etched and rinsed, after which adhesive was applied and light-cured (Figure 3). The restoration for tooth No. 10 was layered as previously described.
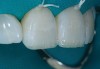
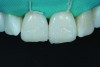
Then, the restorations for teeth Nos. 8 and 9 were created. Minimal augmentation would be required to improve the patient’s smile. The opaque shade was layered slightly irregularly to mimic the appearance of the patient’s natural dentition, particularly the interplay of the enamel and dentin optical properties (Figure 4). A putty matrix was inserted to guide composite placement when augmenting the shape and length of the central incisors using the CL composite (Figure 5). Then, a small amount of CL composite was applied as the final layer (Figure 6) and cured, after which a final polish was performed.
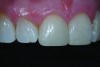
Direct composite bonding allowed this patient to keep tooth No. 10 while improving the overall color, shape, and harmony of teeth in her esthetic zone (Figure 7). Although the results achieved for this patient may not represent ideal esthetic parameters, they did satisfy the patient’s criteria for a minimally invasive yet significant improvement in the appearance of her smile.
Conclusion
Direct composite bonding offers patients many advantages. The choice of improved materials also makes direct bonding effective for dentists to consider when their patients are concerned with maintaining natural tooth structure. In addition, when expense, time, and esthetics are concerns, direct composite bonding procedures are biologically conservative, cost-effective, and painless. For many patients, this treatment can provide almost instant gratification and a treatment modality that can be easily repaired and is highly esthetic. Overall, direct composite restorations may offer patients a non-invasive option for smile enhancements.
About the Author
Abdi Sameni, DDS
Clinical Associate Professor, Ostrow School of Dentistry
University of Southern California
Los Angeles, California
Private Practice
Los Angeles, California
Disclosure
On occasion, Heraeus Kulzer supports Dr. Sameni through sponsorships and material donations.
References
1. DiMatteo A. The smile makeover craze: what it means to you and your patients. Inside Dentistry. 2006;2(4):45-54.
2. Milnar F. Altering tooth inclination and overall esthetics with direct composite veneers, gingival contouring, and enamelplasty. Inside Dentistry. 2006;2(1):46-50.
3. Staehle HJ. Minimally invasive restorative treatment. J Adhes Dent. 1999;1(3):267-284.
4. Mopper KW. Maximizing the potential of composite artistry: three decades of direct resin bonding. Picture Perfect Aesthetics: The AACD Monograph. Vol. II. Mahwah, NJ: Montage Media Corporation; 2005:95-99.
5. Zorba YO, Bayindir YZ, Barutcugil C. Direct laminate veneers with resin composites: two case reports with five-year follow-ups. J Contemp Dent Pract. 2010;11(4):E056-062.
6. Fahl Júnior N. The direct/indirect composite veneers: a case report. Pract Periodontics Aesthet Dent. 1996;8(7):627-638.
7. LeSage B. Challenging the underuse of composites in support of minimally invasive dentistry. Inside Dentistry. 2009;5(1):38-43.
8. Sarver DM. The importance of incisor positioning in the esthetic smile: the smile arc. Am J Orthod Dentofacial Orthop. 2001;120(2):98-111.
9. Ghaleb N, Bouserhal J, Bassil-Nassif N. Aesthetic evaluation of profile incisor inclination. Eur J Orthod. 2011;33(3):228-235.
10. Sarver DM, Ackerman MB. Dynamic smile visualization and quantification: part 1. Evolution of the concept and dynamic records for smile capture. Am J Orthod Dentofacial Orthop. 2003;124(1):4-12.
11. Sarver DM, Ackerman MB. Dynamic smile visualization and quantification: part 2. Smile analysis and treatment strategies. Am J Orthod Dentofacial Orthop. 2003;124(2):116-127.
12. Sarver DM, Profit WR. Special considerations in diagnosis and treatment planning. In: Graber TM, Vanarsdall RL, Vig KWL, eds. Orthodontics: Current Principles and Techniques. 4th ed. St. Louis, MO: Mosby; 2005:18-25, 43-55.
13. McLaren EA, Phong TC. Smile analysis and esthetic design: “in the zone.” Inside Dentistry. 2009;5(7):44-48.
14. Johnston CD, Burden DJ, Stevenson MR. The influence of dental to facial midline discrepancies on dental attractiveness ratings. Eur J Orthod. 1999;21(5):517-522.
15. Shyagali TR, Chandralekha B, Bhayya DP, et al. Are ratings of dentofacical attractiveness influenced by dentofacial midline discrepancies? Aust Orthod J. 2008;24(2):91-95.
16. Bhuvaneswaran M. Principles of smile design. J Conserv Dent. 2010;13(4):225–232.
17. Thomas M, Reddy R, Reddy BJ. Perception differences of altered dental esthetics by dental professioinals and laypersons. Indian J Dent Res. 2011;22(2):242-247.
18. Miller EL, Bodden WR Jr, Jamison HC. A study of the relationship of the dental midline to the facial median line. J Prosthet Dent. 1979;41(6):657-660.
19. Magne P, Gallucci GO, Belser UC. Anatomic crown width/length ratios of unworn and worn maxillary teeth in white subjects. J Prosthet Dent. 2003;89(5):453-461.
20. Lombardi RE. The principles of visual perception and their clinical application to denture esthetics. J Prosthet Dent. 1973;29(4):358-382.
21. Magne P, Belser U. Natural oral esthetics. In: Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing; 2002:84-85.
22. Rifkin R. Facial analysis: a comprehensive approach to treatment planning in aesthetic dentistry. Pract Periodontics Aesthet Dent. 2000;12(9):865-871.
23. Margeas R. Composite resin: a versatile, multi-purpose restorative material. Compend Contin Educ Dent. 2012;33(1):42-45.
24. Bassett J. Conservative restoration of a traumatically involved central incisor. Compen Contin Educ Dent. 2012;33(4):264-267.
25. Fahl N Jr. Optimizing the esthetics of Class IV restorations with composite resins. J Can Dent Assoc. 1997;63(2):108-111, 114-115.
26. Fahl N Jr. A polychromatic composite layering approach for solving a complex Class IV/direct veneer-diastema combination: part I. Pract Proced Aesthet Dent. 2006;18(10):641-645.
27. Chiche GJ, Fahl N Jr, Kois JC. The changing world of dentistry. Dent Today. 2011;30(2):126, 130, 132-133.
28. Gresnigt MM, Ozcan M. Fracture strength of direct versus indirect laminates with and without fiber application at the cementation interface. Dent Mater. 2007;23(8):927-933.
29. Radz GM. Direct composite resins. Inside Dentistry. 2011;7(7):108-114.
30. Jordan RE. Esthetic Composite Bonding. 2nd ed. St Louis, MO: Mosby; 1992.
31. Mitra SB, Wu D, Holmes BN. An application of nanotechnology in advanced dental materials. J Am Dent Assoc. 2003;134(10):1382-1390.